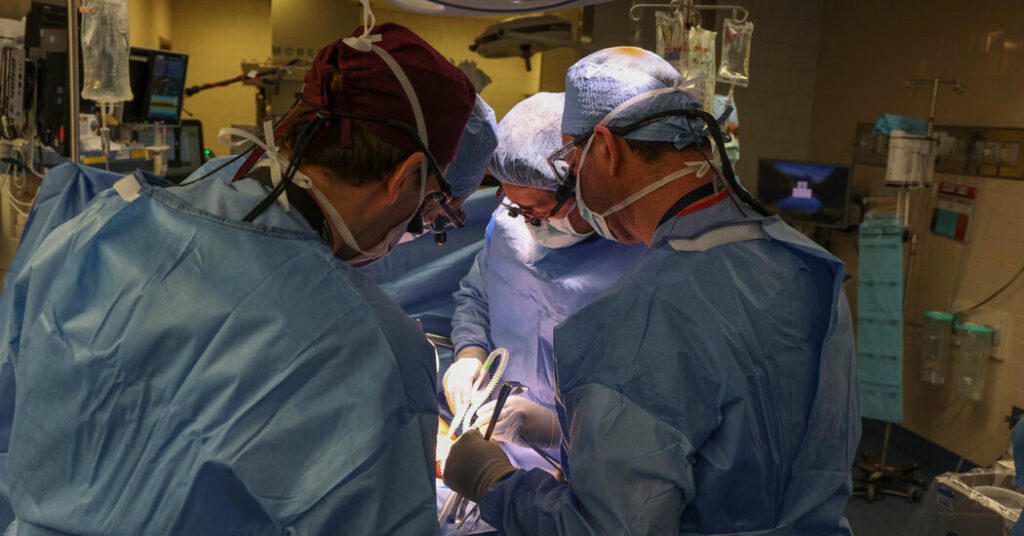
Surgeons in Boston transplanted a genetically engineered pig kidney into a sick 62-year-old man. This is the first surgery of its kind. If successful, this breakthrough could bring hope to hundreds of thousands of Americans whose kidneys are failing.
So far, the signs are promising.
The kidneys remove waste products and excess water from the blood. Doctors at Massachusetts General Hospital say the patient's new kidney started producing urine immediately after the surgery last weekend and his condition continues to improve. He is already walking the hallways of the hospital and could be discharged soon.
The patient was a black man, and the procedure may have special significance for black patients, who have higher rates of end-stage kidney disease.
Winfred Williams, M.D., associate chief of nephrology at Massachusetts General Hospital and the patient's primary care physician, said the new kidney source “could help solve the puzzling problem of minority patients not receiving kidney transplants.” There is,” he said.
If kidneys from genetically modified animals can be transplanted on a large scale, dialysis “will become obsolete,” said Dr. Leonardo V. Riera, medical director of kidney transplantation at Massachusetts General Hospital. The hospital's parent organization, Mass General Brigham, developed the transplant program.
More than 550,000 Americans have kidney failure and require dialysis to filter toxins from the blood. More than 100,000 people are waiting to receive a kidney transplant from a living or dead human donor. End-stage kidney disease occurs three times more often in black Americans than in whites.
Additionally, tens of millions of Americans have chronic kidney disease, which can lead to organ failure.
Dialysis keeps people alive, but the most standard treatment is organ transplantation. However, thousands of patients die each year while waiting for a donated kidney due to a severe organ shortage. Only 25,000 kidney transplants are performed each year.
Xenotransplantation (transplanting animal organs into humans) has been proposed for decades as a potential solution to making kidneys more widely available. However, experts say that long-term rejection can occur even if the donor is well matched, as the human immune system rejects foreign tissue, leading to life-threatening complications.
In recent years, scientific advances such as gene editing and cloning have brought xenotransplantation closer to reality, making it possible to modify an animal's genes to make its organs more compatible and less likely to be rejected by the immune system.
The kidney was taken from a pig that was genetically engineered by biotech company eGenesis to remove three genes involved in the organ's potential rejection. Additionally, he had seven human genes inserted to increase human fitness. Pigs carry retroviruses that can infect humans, and the company has also inactivated the pathogen.
In September 2021, surgeons at NYU Langone Health in New York attached a genetically modified pig kidney to a brain-dead man and watched the kidney begin to function and produce urine. Shortly after, scientists at the University of Alabama at Birmingham announced that they had performed a similar procedure with similar results.
Surgeons at the University of Maryland have twice transplanted genetically modified pig hearts into heart patients. Although the organs functioned and the first organ showed no signs of rejection, two patients with advanced disease died soon afterward.
(Patients who agree to these cutting-edge experimental treatments are usually critically ill and have few options available. They are often too short to join the waiting list for precious human organs.) (They may be too sick or ineligible for other reasons.)
Boston transplant Richard “Rick” Suleiman, a state Department of Transportation supervisor, had long suffered from diabetes and high blood pressure and had been treated at Massachusetts General for more than a decade.
After his kidneys failed, Suleiman underwent dialysis for seven years and finally received a human kidney transplant in 2018. But within five years, her donated organs began to fail and she developed other complications, including congestive heart failure, Dr. Williams said.
When Suleiman resumed dialysis in 2023, he experienced severe vascular complications (his blood vessels clotted and malfunctioned) and required repeated hospitalizations, Dr. Williams said.
Suleiman, who continued to work despite his health problems, faced a long wait for another human kidney and “he became depressed,” Dr. Williams said. “He said, 'We can't go on like this.' This can't continue. I started thinking of special measures we could take.”
“He would have had to wait five to six years to get a human kidney. He would not have survived,” Dr. Williams added.
When Dr. Williams asked Suleiman about donating a pig kidney, Suleiman had many doubts, but ultimately decided to proceed.
“I saw it as a way not only to help me, but also to give hope to the thousands of people who need transplants to survive,” in a statement provided by Mass General. he said.
Suleiman's new kidney appears to be working so far, and he has been able to stop dialysis. The new pig's kidneys produce urine and filter out the waste product creatinine.
Doctors say other measures are improving day by day. Doctors will continue to monitor Mr. Suleiman for signs of organ rejection.
“He looks like himself. It's amazing,” Dr. Williams said.
The surgery was not without its critics. Xenotransplants increase the potential for further exploitation of animals and may introduce new pathogens into the human population, said Kathy Guillermo, executive vice president of People for the Ethical Treatment of Animals.
“Using pigs as a source of spare parts is dangerous for human patients, deadly for animals, and could spark the next pandemic,” she said. “It is impossible to eliminate or even identify all the viruses pigs carry. Researchers need to focus on cleaning up the organ donation system and leave the animals alone.”
The four-hour surgery was performed by a team of surgeons including Dr. Tatsuo Kawai and Dr. Naher Elias, director of the Legorreta Clinical Transplant Tolerance Center in Massachusetts.
The procedure was carried out under a Food and Drug Administration protocol known as the “compassionate use provision,” which allows patients with life-threatening illnesses who could benefit from unapproved treatments. New drugs to suppress the immune system and prevent organ rejection were also used under this protocol.
Dr. Williams said of Mr. Suleiman, “He is incredibly courageous in stepping forward.” “Hats off to him. He's made a huge contribution to this.”