Tablets to be taken once a week. Inject at home once a month. Even with the jab given in clinic every six months.
Within the next 5 to 10 years, these options may become available for HIV prevention and treatment. Scientists are getting closer to developing longer-acting alternatives to drugs that must be taken daily. Perhaps even a future will come true in which HIV requires attention only twice in a year. It was an unimaginable year in the darkest decades of this epidemic.
Mitchell Warren, executive director of HIV prevention group AVAC, said: “This period is the next wave of innovation, with new products emerging to meet people's needs in ways never seen before, particularly in the field of prevention.” Stated.
Long-acting treatments may eliminate the need to remember to take daily medications to prevent or treat HIV. And for some patients, new drugs may reduce the stigma of the disease, which itself is an obstacle to treatment.
“For them, it means they don't have to be reminded that every morning is about changing the planet,” said Rachel Bender Ignacio, director of UW Positive at the University of Washington, a clinical research site focused on HIV. the doctor said. That's what prevents them from taking it every morning. ”
Long-acting drugs could be an even bigger boon for people who have long had difficulty obtaining them. These include patients who have unstable access to medical services, patients who have difficulty taking their medications every day due to unstable housing or transportation, and patients who have difficulty taking drugs. Are mentally ill or face discrimination or prejudice.
In 2022, nearly 30 years after the advent of combination antiretroviral therapy, more than 9 million of the 39 million people living with HIV worldwide are not receiving treatment. In the same year, approximately 630,000 people died from AIDS-related illnesses.
In the United States, about one-third of people diagnosed with HIV are unable to suppress the virus. “We still haven't addressed these fundamental questions of access,” said Greg Gonsalves, a longtime HIV activist and epidemiologist at the Yale School of Public Health.
He added that “we can be overjoyed about the science and clinical impact” of longer-lasting drugs. “But for many, that will be a distant dream.”
One barometer of the excitement for long-acting regimens was their prominence at the Retroviruses and Opportunistic Infections Conference in Denver in March. The annual conference has served as the backdrop for many HIV milestones, including the shocking moment in 1996 when researchers showed they could suppress the virus with a combination of drugs.
Dozens of studies on long-acting regimens were presented at this year's conference. (Most such drugs are very close to preventing and treating HIV, but similar options for tuberculosis, hepatitis B, and hepatitis C are not far behind.)
One long-acting treatment, Cavenuva, is given in two doses every other month and has been available for nearly three years. It costs more than $39,000 a year in the United States, but few patients pay that amount. But even with deep discounts, this treatment remains out of reach for many patients in low-income countries.
Still, many researchers at the conference cited the results of one study showing Cavenuva to be more effective at controlling HIV than daily pills, even in groups that typically have difficulty adhering to treatment. I was excited.
“Given how difficult it is for some people, it's really important that we have new tools that could potentially keep them in check,” said Kimberly Smith, head of research and development at ViiV Healthcare. the doctor said. One of the component drugs of Cabenuva.
Long-acting drugs may also help children living with HIV Globally, only about half of children diagnosed with HIV receive treatment.
Part of the reason is a lack of medicines made for children, Dr. Charles Flexner, an HIV expert at Johns Hopkins University, said in a presentation at the Denver conference.
“With long-acting formulations, that's no longer the case,” Dr. Flexner says. “Children will be able to use the same formulation as adults, just at different doses.”
Most long-acting shots contain nanocrystals of the drug suspended in a liquid. While oral tablets must pass through the stomach and intestinal tract before entering the circulation, so-called depot shots deliver the drug directly into the bloodstream. However, they are released very slowly, over weeks or months.
Some depot antipsychotics are given every 2 to 8 weeks, and the birth control pill Depo-Provera is given once every 3 months. Cabenuva — a combination of cabotegravir manufactured by Viiv Healthcare (majority owned by GSK) and Janssen's rilpivirine — is injected into the buttock muscle every two months to treat HIV.
Cabotegravir given subcutaneously in the stomach caused more bruising and rashes than in the buttocks, and some people developed nodules that lasted weeks or even months. But with injections in the buttock, “there's nothing visible,” Dr. Smith said. “You may feel pain for a few days, but then you can go on with your normal life.”
Viiv is developing a version of cabotegravir that would be administered every four months and eventually every six months. The company aims to bring a four-month version to market for HIV prevention in 2026 and for treatment in 2027.
But for people with high body fat or silicone implants in their buttocks, like some trans women, injecting drugs into their muscles is difficult. Some new shots in development are administered under the skin to avoid the problem.
Gilead's lenacapavir can be injected subcutaneously into the stomach once every six months, but so far it has only been approved for people with HIV who are resistant to other drugs. The drug is in multiple late-stage trials as a long-acting HIV prevention drug in various groups, including cisgender women.
Lenacapavir is also being tested as a once-weekly pill treatment in combination with another Merck drug, islatravir. “Ideally, we would have multiple long-acting treatments so people can actually choose between the options that are most effective for them,” said Dr. Jared Baeten, vice president of Gilead. Ta.
Santos Rodriguez, 28, was diagnosed with HIV in 2016 and has been taking daily medication ever since to suppress the virus. Having to take just one pill a week is “definitely a game changer for me and for compliance,” said Rodriguez, who works in artificial intelligence research at the Mayo Clinic in Florida.
He said he was reluctant to get the Cavenuva injection because it requires clinic visits every two months and there have been reports that the buttock injections are painful. A shot every four months or every six months would be much more attractive, he added.
To truly make it available to everyone, including those who live far from medical centers, researchers also need to create long-acting injectables that can be self-administered. some experts point out.
One team is developing just that and plans to make it available to low- and middle-income countries with support from global health initiative Unitaid.
“What's really interesting about this is that this method of development ideally avoids the trickle-down effect and gets it to the people who need it most,” said Dr. Bender-Ignacio, referring to trends in rich countries. . First, you will have access to new treatments. She is leading the research.
This product uses a lipid base to suspend three HIV drugs (two water-soluble and one fat-soluble). Unlike depot shots, which release the drug slowly, these so-called nanolozenges are delivered subcutaneously in the stomach and immediately taken up by immune cells and lymph nodes.
Dr. Bender-Ignacio said this efficiency allows the shot to deliver a smaller dose of drug and make it easier to adapt to children and adolescents. One injection allows him to maintain levels of the three drugs in his body for more than a month, which is the equivalent of 150 tablets.
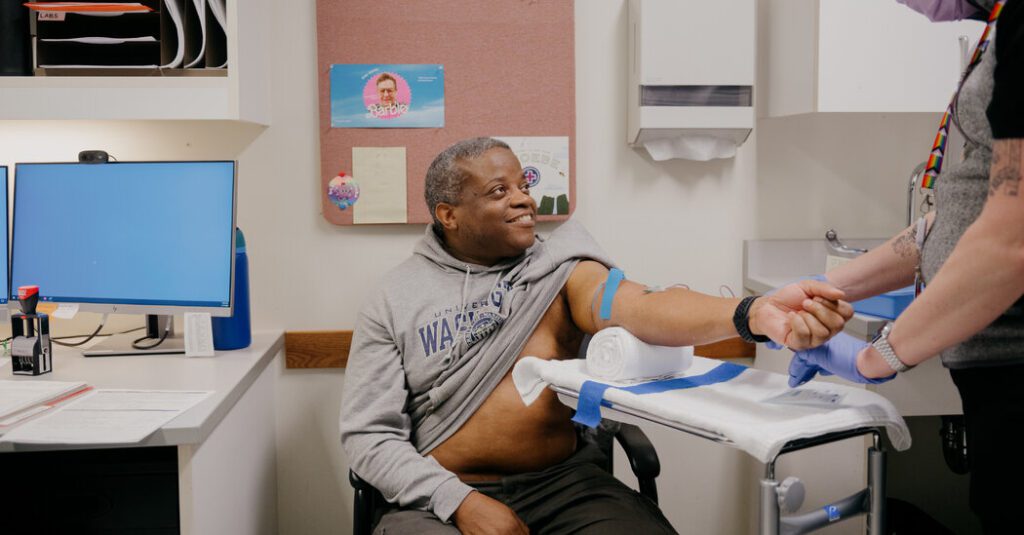
So far, only 11 people have been tested for the self-administered long-acting syringe, including Kenneth Davis, 58, of Auburn, Washington. Sting – temporary and less painful than the COVID-19 vaccine.
Because the component drugs are independently approved, Dr. Bender-Ignacio estimated that these vaccines could be available to treat HIV within five years.
Many of the products, including those included in Dr. Bender-Ignacio's research, can be tailored to prevent HIV. There are currently only three options: two daily pills and ViiV's cabotegravir, which is injected into the buttock every two months.
“For the past 10 years, the slowest response to AIDS has been prevention,” AVAC's Warren said.
One study presented at the Denver conference showed that when people were offered a choice of prophylaxis, more chose long-acting cabotegravir. However, the proportion choosing to take the pill daily also increased.
“The fact that we're seeing increased protection in a variety of ways, that's the most important thing to me,” Warren said. The study “actually shows that there is evidence behind the choices, not just advocacy,” he added.