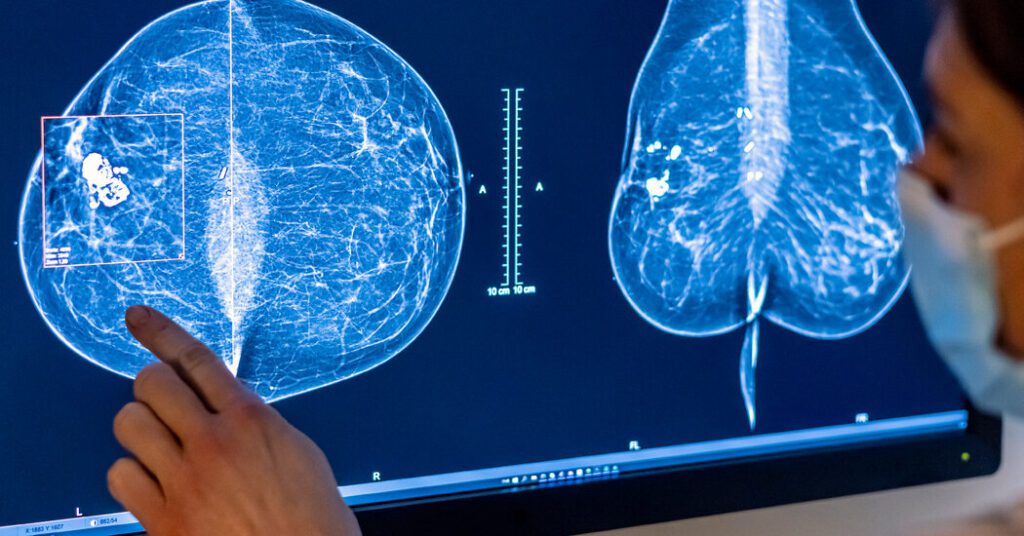
An expert panel on Tuesday recommended that most women start getting regular mammograms at age 40, overturning a long-standing controversial guideline to wait until age 50, citing rising breast cancer rates among young women. .
That committee, the U.S. Preventive Services Task Force, finalized draft recommendations released last year. This group publishes influential advice on preventive health, and its recommendations are typically widely adopted in the United States.
In 2009, a task force raised the age for starting routine mammography from 40 to 50, sparking widespread controversy. At the time, researchers found that early screening can do more harm than good and lead to unnecessary treatments in young women, including a surprising finding that could lead to invasive but ultimately unnecessary anxiety-inducing procedures. I was worried that this might happen.
However, the incidence of breast cancer among women in their 40s is currently on the rise, increasing by 2% annually from 2015 to 2019, said Dr. John Wong, vice chairman of the task force. Although many patients and health care providers prefer annual screening, the panel continues to recommend screening every two years for women at average risk for breast cancer.
“There is clear evidence that biennial screenings starting at age 40 provide significant benefits, so screening should be encouraged for all women in this country to live longer and improve their quality of life. ” said Dr. Wong of primary care. She is a clinician at Tufts Medical Center and director of comparative effectiveness research at the Tufts Institute for Clinical and Translational Sciences.
The recommendation faced harsh criticism from some women's health advocates, including Rep. Rosa DeLauro, D-Connecticut, and Rep. Debbie Wasserman Schultz, D-Florida, who said it did not go far enough. has been done.
In a letter to the task force in June, they said the guidance continues to “fall short of science, create coverage gaps, create uncertainty for women and their health care providers, and exacerbate health disparities.” It's making it worse.”
Refocusing on a hotly debated topic, the panel also said there was not enough evidence to support additional tests such as ultrasound or magnetic resonance imaging for women with dense breast tissue.
This means that insurance companies do not need to universally offer additional screening to these women, who are at high risk for breast cancer in the first place because mammography alone can miss the cancer. Approximately half of women over 40 fall into this category.
In recent years, more mammography providers are required by law to notify women if their breast tissue is dense and to tell them that mammography may be an inadequate screening tool for them.
Starting in September, all mammography centers in the United States will be required to provide that information to patients.
Doctors often prescribe additional or “supplementary” scans for these patients. However, these patients end up having to pay all or part of the cost themselves, even when additional tests that should legally be provided free of charge are performed as part of preventive treatment. often noticed.
Medicare, the government's health insurance plan for older Americans, does not cover the additional tests. In the private insurance market, coverage is dispersed depending on factors such as state law, plan type, and plan design.
The Special Committee sets standards that must be covered by law for preventive health services that health insurance companies can provide to patients free of charge.
Robert Traynham, a spokesman for AHIP, an association representing health insurance companies, said the committee's decision not to support additional testing has significant implications for patients.
“What this means for insurance coverage is that there is no obligation to cover these specific tests for women with dense breasts at no cost to them,” she said.
While some employers may choose to do so for their health insurance plans, it is not required by law, Traynham said.
Kathleen Costello, a retired Southern California retiree who was diagnosed with breast cancer in 2017 at age 59, said she believes mammograms have missed the cancer for years.
She was tested every year and received a letter every year saying she was cancer-free. Her letter also told her that her breast tissue was dense and that additional tests were available but would not be covered by insurance.
In 2016, six months after her mammogram came back normal, she told her doctor that her right breast felt firm. The doctor ordered a mammogram and an ultrasound.
“We found the cancer within 30 seconds of the ultrasound,” Costello said in an interview, adding that he found out because “the technician turned pale and left the room.”
Mr Costello added that the mass was 4cm in size, adding: “To go from undetectable to 4cm in six months is unacceptable to me.” .
However, Dr Wong of the task force said there is no scientific evidence to prove that supplementary imaging with MRI or ultrasound can slow the progression of breast cancer or extend the lifespan of women with dense breast tissue.
On the other hand, there is ample evidence that additional screening can lead to frequent false-positive findings and biopsies, contributing to stress and unnecessary invasive procedures.
“It's tragic,” Dr. Wong said. “We're just as frustrated as women. They have a right to know whether additional screening would help.”
However, medical organizations like the American College of Radiology recommend additional screening for women with dense breast tissue. Dr. Stamasia Destonis, chair of the university's breast imaging committee, said research shows that mammography and ultrasound can be used together to detect additional cancers in patients with dense tissue.
Dr. Detounis said that recent studies have shown that MRI is the best adjunct scan for women with dense breasts who are at average risk for breast cancer, and that it provides “much better cancer detection and better “We can get a positive predictive value.”
The university also recommends that women at average cancer risk be screened annually, rather than every two years as recommended by the committee. A group of radiologists has called for a recommendation that all women should be assessed for breast cancer risk before the age of 25, so that high-risk women can start screening before the age of 40. .
There is growing evidence that black, Jewish and other ethnic minority women develop breast cancer and die from breast cancer more often before age 50 than other women, Dr. Detounis noted.
Trans men who haven't had a mastectomy should continue to be screened for breast cancer, she said, and trans women, whose hormone use puts them at higher risk of breast cancer than the average man, should discuss screening with their doctors. added.
While the committee's recommendation to start testing at age 40 is an “improvement,” the final recommendation “is not enough to save women's lives,” Dr. Detounis said.